How to Check an Infant for a Lip-Tie and Tongue-Tie Properly
Many dentists are asked to evaluate infants for a lip-tie or tongue-tie by concerned parents, but we were never trained in school how to do this. Although it’s too much to cover in one post, I’ll give you the highlights.
The first key to treatment is there has to be a problem. We don’t release a tongue or lip-tie unless there is a feeding or medical concern. The related issues are more far-reaching than you probably think though!
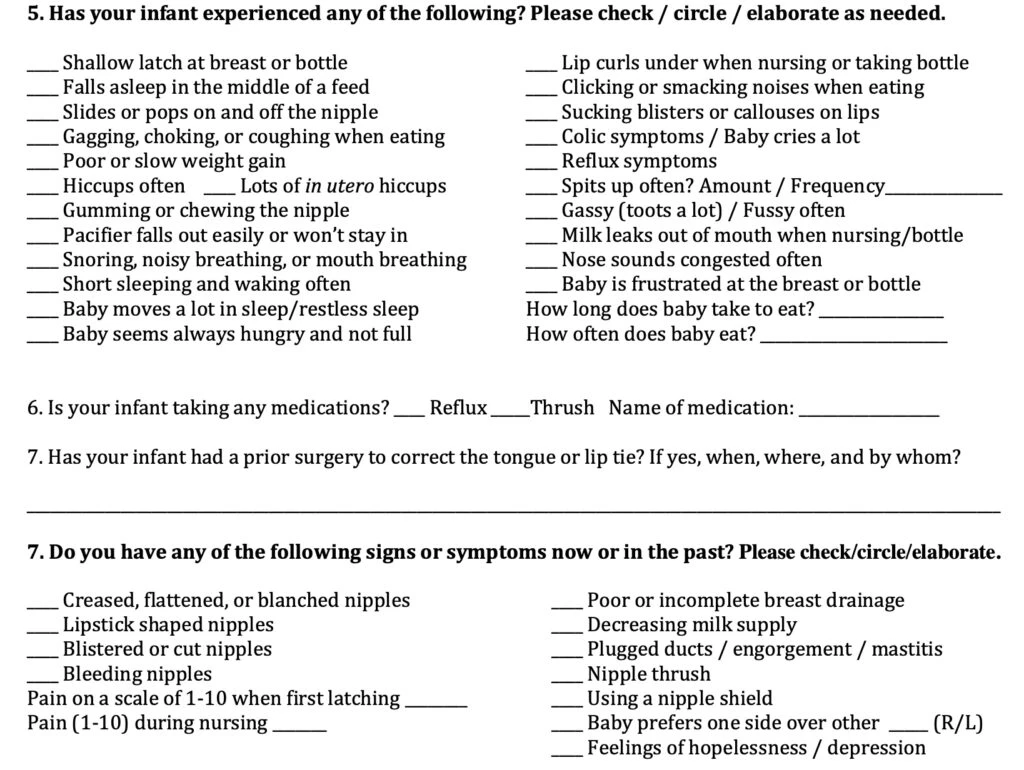

Nursing pain and poor weight gain are certainly two of the biggest issues that arise, but we have many struggling babies who are bottle-feeding or have excellent weight gain, and still have problems worth addressing. So we use an infant assessment sheet like this one to see what the related issues are. If a mom has more than a few checkmarks on this form, have a high degree of suspicion for an oral restriction.
Slow eating, constantly hungry, fussy, gassy (moms say “he toots like a grown man!”), spits up often, reflux, can’t hold a paci, or mom has nipple pain or distortion (flattened, lip-stick shaped nipples, etc.), and needing a nipple shield, mastitis, plugged ducts, can all be related to a tongue/lip-tie.
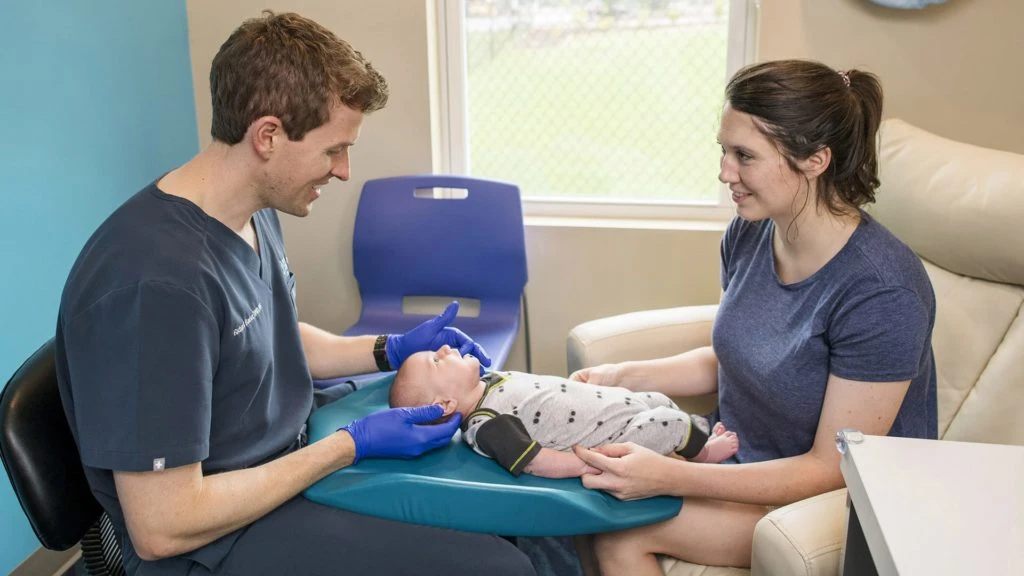
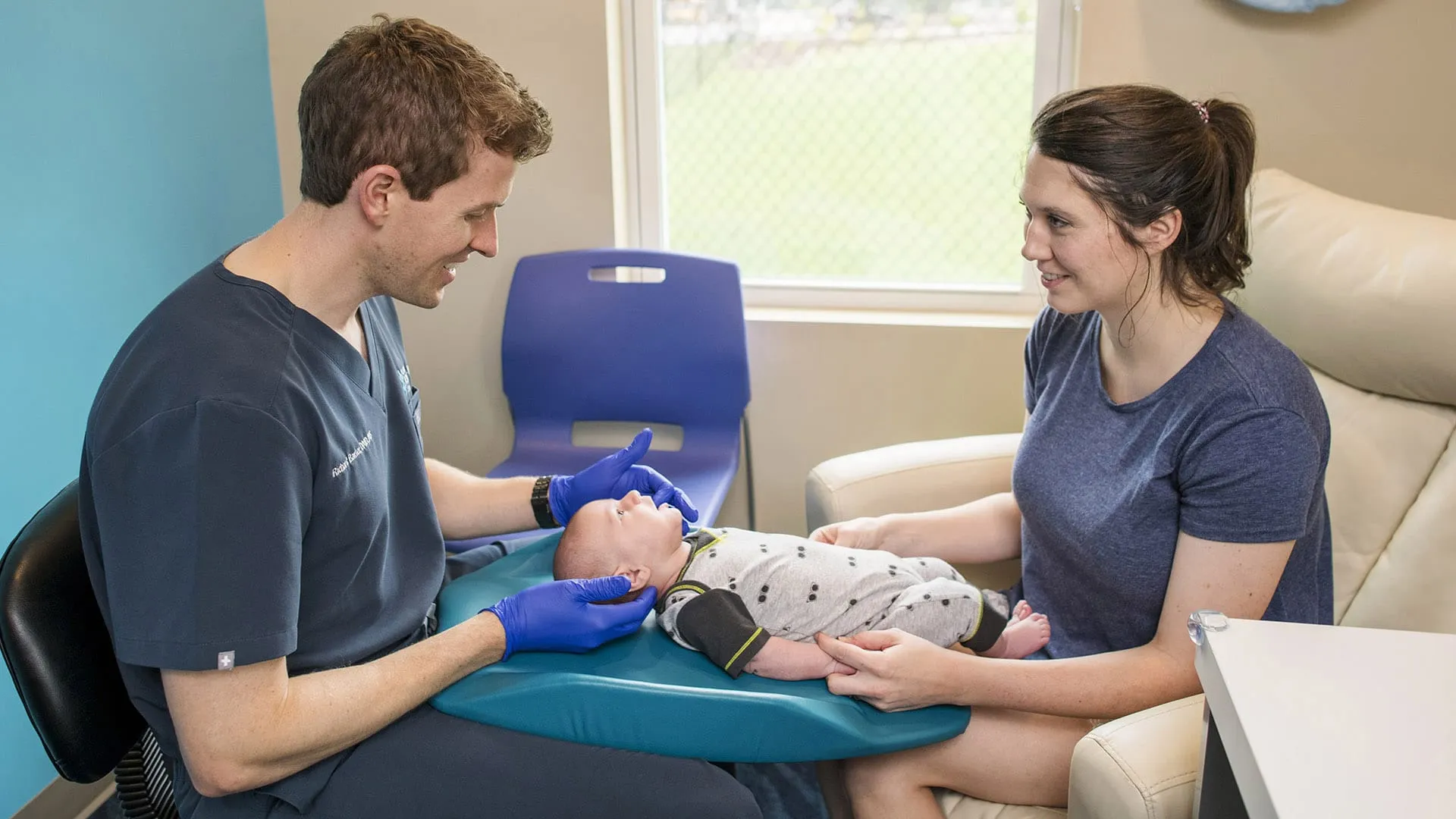
To properly assess an infant, the baby needs to be placed on an exam table, dental chair, or lapboard. The baby cannot be in a car seat, mother’s arms, or checked without putting on gloves. Come from behind to lift the lip and check for blanching of the tissue, distress or discomfort from lifting the lip, and check the attachment location… but primarily feel for tension. Then check the cheeks for buccal (pronounced “buckle”) restrictions, it feels like a speed bump or guitar string up in the cheek vestibule. We occasionally treat buccal ties, maybe 10% of the babies we see. There’s just a lack of research on those, so we leave it up to the parents’ decision.
Then we come from behind and elevate the tongue with two index fingers, one on each side of the frenum, and lift. You can see the tension get tighter as you lift the frenum as the fascia bunches up into a string. If it is not easily visible at first, this could be a submucosal webbing of fascia that is still restricting function (a posterior tongue-tie, as discussed last week).
Interestingly and unfortunately, for the moms who report the worst nursing pain, often the tongue-tie is less obvious, or posterior (and often not picked up by healthcare providers). But when treated, they very often have immediate relief of nursing pain, while still in the office.
We’ll go more into detail next week. In the meantime, if you’re a patient and think your child may have a tongue-tie or lip-tie, please call us at 205-419-4333 or contact us to schedule a consultation. If you’re a professional, and you’d like to download our infant forms so you can help treat infants struggling with tongue-tie issues, or learn more, visit our page for Professionals.