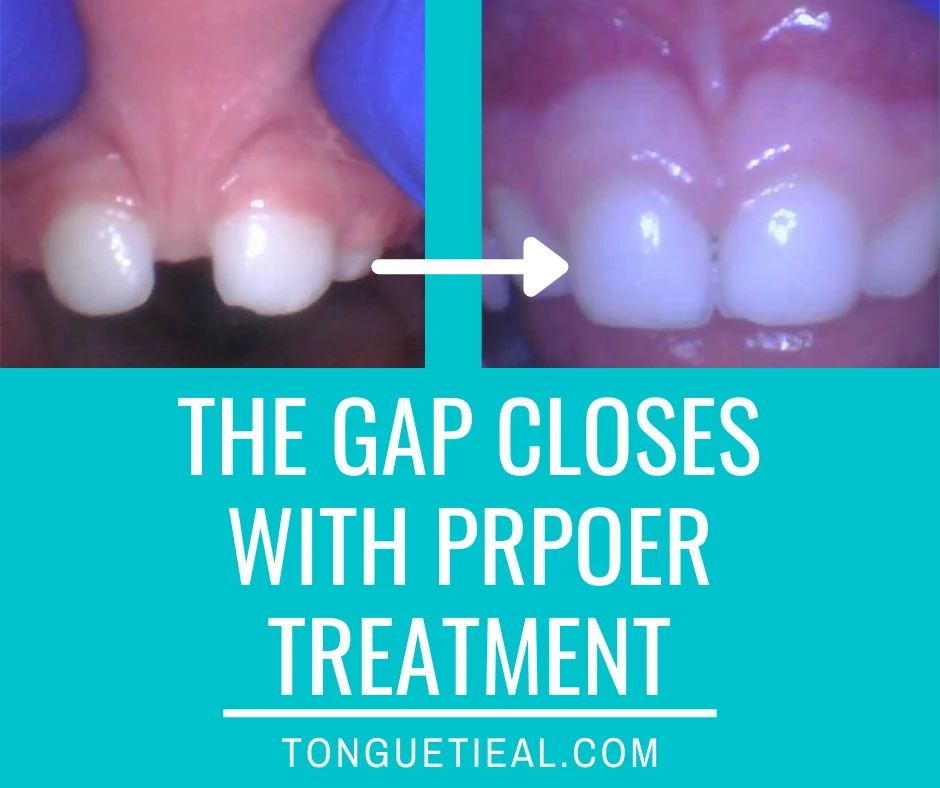
Is it safe to treat a lip tie early? Does early treatment of a lip tie prevent gap closure? Does it help the gap close?
These are common questions in pediatric dental practices across the country. Clinically, we see the answer to these questions on a daily basis in patients we treated for a lip tie several years earlier when they were a baby or a toddler (or adolescent). When the lip tie is properly removed (not just a clip or snip with scissors), the gap closes up almost always (94% of the time). It at the very least decreases in size, typically to a normal width that is much more likely to close spontaneously in the future.
The main reasons we treat lip ties are for breastfeeding and related issues (poor seal on the bottle or breast, which leads to air swallowing, which leads to gas, colic, reflux, etc.) as well as toddlers with issues with oral hygiene (they fight when brushing the top teeth), issues with B, P, M, and W sounds (bilabial sounds), and cosmetic concerns (you can’t see their teeth when they smile, or a large gap in the teeth). The procedure is quick, has minimal risks, and high satisfaction from parents. The only issue is that other providers think there will be “scar tissue” that will prevent the gap from closing when they try to do braces ten years later.
So a few years ago, we set out to quantify this closure and assess the risk of the gap not closing after treatment. We took every patient we had ever treated for lip tie and tried to get as many post-op pictures as we could when they came back for their cleaning, fillings, or we just emailed, called, and texted parents to see if they could send us a close-up photo of their child’s teeth. We take before photos of every lip or tongue-tie we treat, so we could use our x-ray software to digitally measure the gap before the procedure, and use that same software to measure the gap after the procedure. This is the first study to ever look at this question years after performing a frenectomy, fully removing the restricted tissue, and measuring the gap digitally after time has passed to note the changes.
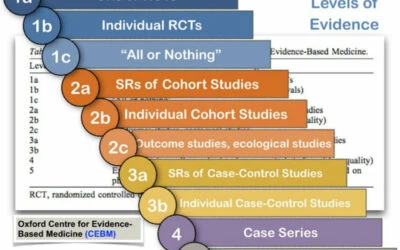
What we found goes against what is taught in pediatric dental and orthodontic programs. So when we try to submit the data, they don’t want to publish it because they have a confirmation bias to go with what has already been published. This is a big problem in research. People want to accept research that goes along with their preconceived ideas of what is correct and deny research that challenges these long-held assumptions. The concept that early treatment of a lip tie would cause “scar tissue” that would prevent gap closure was proposed by Bishara in 1972 (so 50 years ago) who said that you should close the space with braces first, then treat the lip tie. Because of that one opinion piece (there was no patient data to back up his claim) then all the textbooks said “this is the order: braces first, then lip tie.” So that’s what is taught.
Here are some data backing up our claim. 94% of the time, a year or two later, the gap closed up. Scar tissue did not form when it was treated before braces. Most (75%) of the treated kids are unlikely to need braces for a gap in their teeth because now their gap is to a “normal size” of less than 2mm. This is from our abstract.
In total, 109 patients were included: 95 patients with primary dentition (39% male; mean age 1.9 years +/- 1.5 years) and 14 with mixed dentition (43% male; mean age 8.1 +/- 1.3 years) with a mean follow-up of 18.0 ± 13.2 months. No adverse outcomes were noted other than minor pain and swelling. In the primary dentition, a decrease in diastema width was observed in 94.7% with a mean closure of -1.4 ± 1.0mm (range +0.7 to -5.1mm). In the mixed dentition, a decrease in diastema width was observed in 92.9% with a mean closure of -1.8 ± 0.8 mm (range 0 to -3.5 mm). 74.5% of patients in the primary dentition and 75% of patients in the mixed dentition with preoperative diastema > 2mm improved to < 2mm width postoperatively.
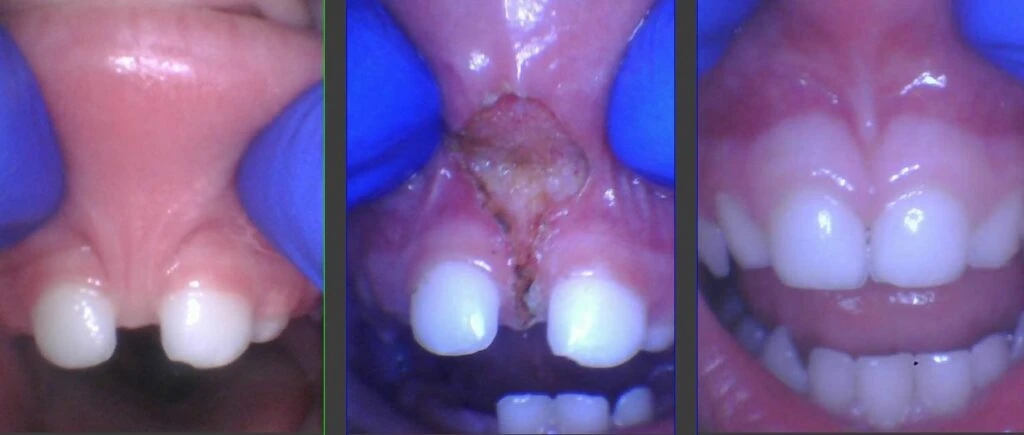
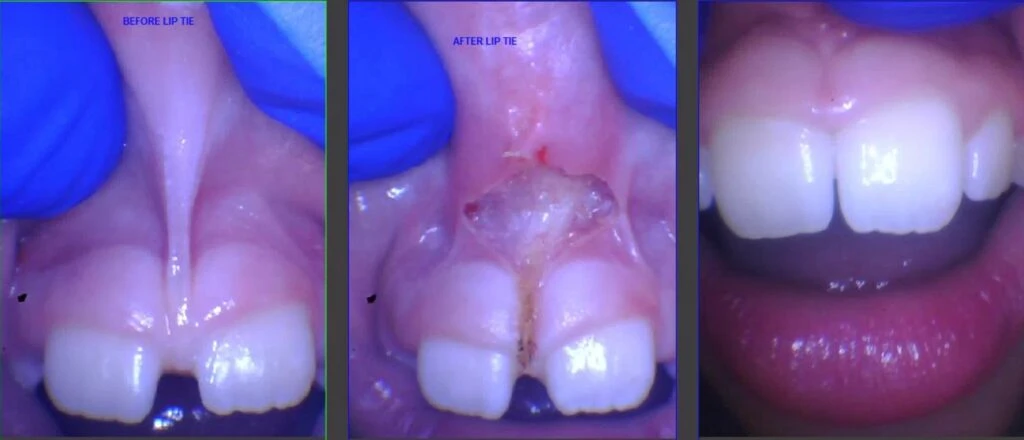
For those still unconvinced, here are some images of how the gap can close on its own without braces if it is treated properly. We do not sedate or even use nitrous on these patients. Younger children get compounded topical, and older children receive injected lidocaine as well. The procedure is completed with a CO2 laser in about 15 seconds with minimal bleeding, and most are completely bloodless. The tissue heals up in about 3 weeks, but is only a little sore for a few days. Stretches are necessary to prevent regrowth of tissue for that time. Parents are often pleased with how much better their child can smile, make sounds, and how much easier it is to brush their child’s teeth after it heals.
If you would like to have your child evaluated for a lip tie, you can call to schedule an evaluation at 205-419-4333, or send us a message. If you are a provider and would like to learn how to perform the procedure, check out our comprehensive online course, Tongue-Tied Academy.
We are in the process of submitting the article for peer review and hope to have it published as soon as possible to combat uninformed recommendations that are based on 50-year-old opinions with decisions based on clinical patient data. Here’s the article abstract:
Background
Maxillary labial frenectomy in children is a common procedure, but concerns about scar tissue formation affecting diastema closure prevent many clinicians from treating prior to orthodontics.
Material and Methods
Pediatric patients with hypertrophic maxillary frena were treated under local anesthesia with diode laser and CO2 laser. The width of the diastema was compared by calibrating and digitally measuring initial and postoperative intraoral photographs.
Results
In total, 109 patients were included: 95 patients with primary dentition (39% male; mean age 1.9 years +/- 1.5 years) and 14 with mixed dentition (43% male; mean age 8.1 +/- 1.3 years) with a mean follow-up of 18.0 ± 13.2 months. No adverse outcomes were noted other than minor pain and swelling. In the primary dentition, a decrease in diastema width was observed in 94.7% with a mean closure of -1.4 ± 1.0mm (range +0.7 to -5.1mm). In the mixed dentition, a decrease in diastema width was observed in 92.9% with a mean closure of -1.8 ± 0.8 mm (range 0 to -3.5 mm). 74.5% of patients in the primary dentition and 75% of patients in the mixed dentition with preoperative diastema > 2mm improved to < 2mm width postoperatively.
Conclusions
Frenectomy is associated with cosmetic and oral hygiene benefits and when performed properly, does not impede diastema closure and may help aid closure. The procedure is performed under local anesthesia with minimal side effects. Technique and case selection are critical to successful outcomes.